Surgical Case of the Month (for Doctors)
Case Study #1: Gum Depigmentation
View Full Case StudyChief Concern: Our 32-year-old female patient was very unhappy with the discoloration of her gums and wanted to feel more confident with her smile. Physiologic pigmentation was present in a random pattern.
Treatment Received: Using the Millenium MVP-7 laser, Dr. Fava treated the gingival pigmentation by removing the melanocytes in the basal lamina. These melanocytes replicate with very low frequency. The laser treatment is therefore considered superior to bleaching, a process which allows melanocytes to continue to produce pigment.
The patient was ecstatic with the outcome and comfort level.
*Click Here for Full Clinical Case with Treatment Details.
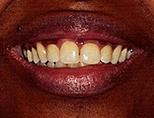

Before Treatment
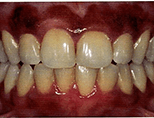
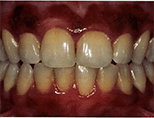
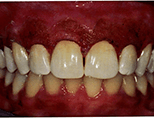
After Treatment
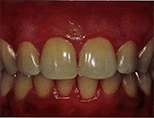
Case Study #2: Alison K.
View Full Case StudyChief Concern: In this esthetic zone, single immediate -implant case, a healthy 45-year-old female (ASA II) required pretreatment of a failed maxillary central incisor (#9) due to severe internal-external root resorption.
Treatment Received: Immediate extraction of #9 was followed by immediate implant placement using an anatomically correct surgical guide along the palatal wall. Buccal gap was bone grafted with a slowly resorbing bone graft. Palatal CTG was placed in the envelope flap to the MGJ under buccal flap (provisional restoration now became a 2-unit cemented cantilevered acrylic bridge #8-9x (pontic).
*Click Here for Full Clinical Case with Treatment Details..
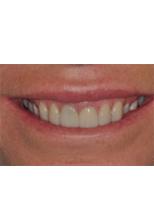

Case Study #3: Alison
View Full Case StudyChief Concern: A healthy, 31-year-old female (a non-smoker) came to our office to consult about the “gummy smile” she wanted to correct. An FMX with vertical bitewings and routine clinical pictures were taken to determine the classification of Altered Passive Eruption (APE): Type 1 (excessive attached gingiva) or Type 2 (lacking attached gingiva) along with the location of the osseous crest: subgroup A: osseous crest is in a normal position to the CEJ with room for the “biologic width” or subgroup B: osseous crest is at the osseous crest (more difficult to treat as significant ostectomy is needed to provide for the “biologic width”- gingival relapse will occur if not diagnosed).
Treatment Received: A buccal approach was made using submarginal incisions made to the cEj followed by full thickness flaps. Significant buccal and interproximal osseous ledges and bony thickness was reduced with speed burs and Piezosurgery ® crown lengthening inserts. This causes the lip to relax and move coronally, creating a “lip repositioning.” Osseous crown lengthening from DB to MB line angles as needed. A Millennium® NdYAG maxillary frenectomy was completed. Suturing with 6-0 polypropolene (anterior papillaes) and 4-0 chromic gut (posteriors). Post-operative visits were suggested for coronal polishing as well as a plaque control review every three weeks for three months with a registered dental hygienist.
*Click Here for Full Clinical Case with Treatment Details.


Case Study #4: Candace
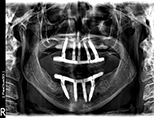
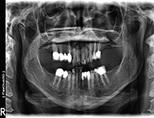
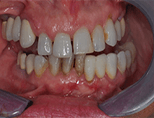
View Full Case StudyChief Concern: 65-year-old (non-smoker) female came to our practice to request a third opinion regarding the ideal treatment for her failing dentures, re-incurring cavities (resulting from medically-induced dry mouth, and acute chronic periodontitis). Her main priorities were to achieve a permanent solution which would provide better comfort and a more esthetically pleasing smile.
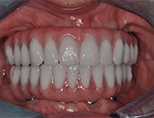
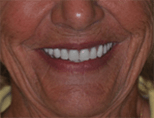
Treatment Received: In one surgically-coordinated visit with us and prosthodontist Dr. Harry Randel, all remaining teeth were extracted. Significant vertical ridge height reduction was then completed to provide the necessary prosthetic room for a hybrid restoration. Five dental implants were placed in the upper jaw, and four implants were placed in the lower jaw. The following day, a screw-retained metal-reinforced fixed provisional prosthesis was put in place. In three months, after full bone healing was confirmed, permanent screw-retained restorations were put in place.
*Click Here for Full Clinical Case with Treatment Details.
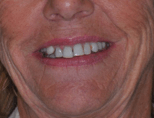
Before Treatment

After Treatment